Chronic Pain, Opioids, and Suicide
/A study covering 18 states raises concerns that chronic pain may be a risk factor for suicide.
This week – is chronic pain a risk factor for suicide as we examine this study appearing in the Annals of Internal Medicine.
Chronic pain is widespread in the US with most studies suggesting a prevalence of around 10% among adults. For health care providers, chronic pain is frustrating. We have limited effective therapies and patients have limited ability to access those therapies. For many of us, the chronic back pain our patient complains of goes to the bottom of the problem list, to be dealt with when, and if, we can get the “more important issues” cleared up.
The Annals paper suggests that we need to be taking chronic pain more seriously though, going so far as to state explicitly that “chronic pain might be an important risk factor for suicide”.
The study identified 123,000 individuals who died by suicide from the National Violent Death Reporting System which had data from 18 states. They then analyzed each record to determine if the individual had chronic pain.
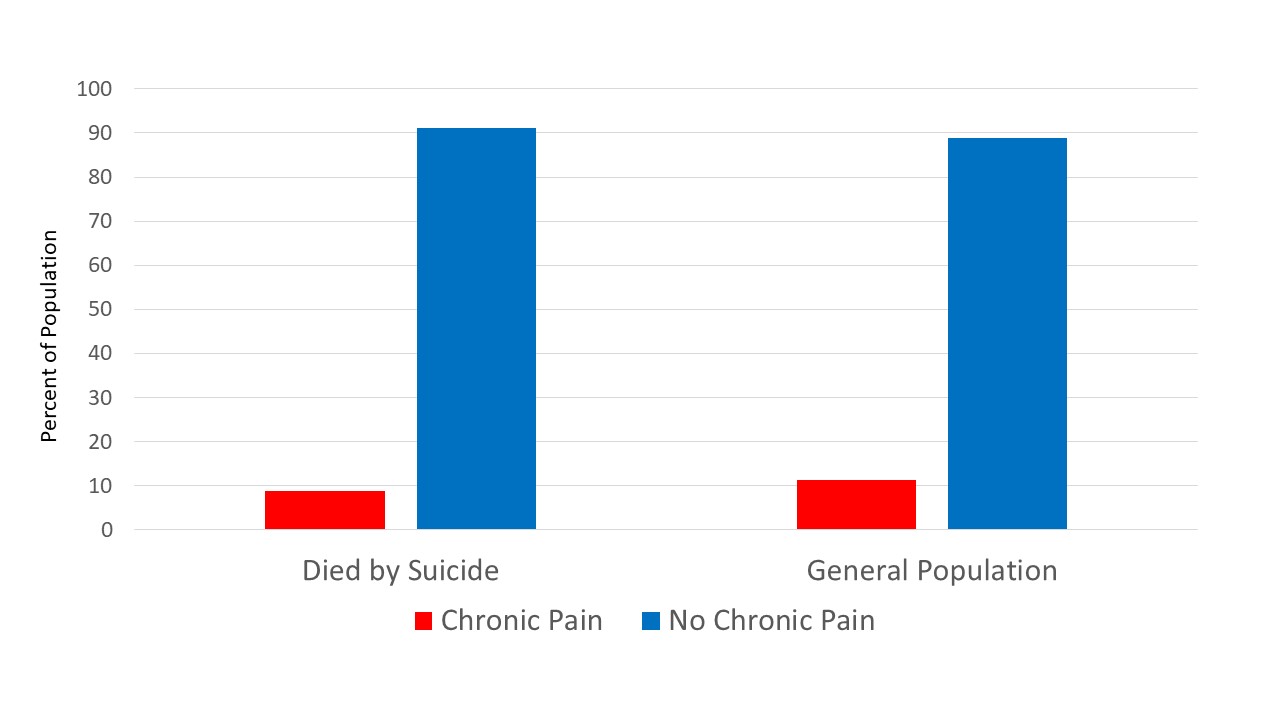
8.8% did.
Let’s stop there for a moment. While this data shows us that some people who die from suicide have chronic pain, that percentage seems pretty similar to the overall percent of Americans who have chronic pain.
Is chronic pain a risk factor, or is it just the background noise of modern society?
I asked the study’s lead author Emiko Petrosky, a Medical Epidemiologist with the Centers for Disease Control. She pointed out that in US survey studies, researchers can simply ask if an individual has chronic pain,
“But for us, we’re not able to ask the person directly. It’s very possible that people had chronic pain but either their loved ones didn’t realize how much it affected them or the loved ones didn’t disclose that pain was a factor in the suicide.”
In other words, 8.8% may be a serious underestimation.
Which leads to some interesting questions. I found myself focusing quite a bit on opioids.
Every time I talk about the opioid epidemic and how physicians should be careful prescribing opioids for chronic pain, I get a significant backlash from patients with chronic pain and their providers who feel that opioids are the only thing keeping patients from suicide.
This concern is actually supported by the researcher’s analysis of 95 suicide notes from individuals with chronic pain. 64 of those notes stated pain played a role in their decision to die by suicide. This is chilling and heartbreaking data.
On the other hand, access to opioids provides a suicide method. Indeed 16.2% of the individuals with chronic pain died from opioid overdose, compared to just 3.9% of those without chronic pain.
Does chronic pain cause suicide? The study can’t tell us for sure, but there are some hints it may play such a role. For example, individuals who died from suicide with chronic pain were less likely to have other suicide triggers like a problem with an intimate partner, a recent argument, or a life stressor. In other words, chronic pain may reduce the threshold for suicide.
Taken together, Dr. Petrosky says one conclusion is clear:
“It is essential that we improve chronic pain management through integrated patient-centered pain management that includes behavioral and mental healthcare in addition to medication for these patients.”
If you need help for yourself or someone else, please contact the National Suicide Prevention Lifeline Talk: 1-800-273-TALK (8255). Chat: www.suicidepreventionlifeline.org
This commentary first appeared on medscape.com.