Spike in Hepatitis C Infections May Be Side-Effect of Oxycontin Reformulation
/In 2010, oxycontin was reformulated to deter abuse. There may have been some nasty side-effects to that change.
Take a look at the incidence of Hepatitis C infection in the US over time.
(Arnold voice): Your hopes of abusing oxycontin have been… crushed.
We’d been doing all right until around 2010, when the rates started to increase. What happened in 2010?
Well, a lot of things.
Christoph Waltz won the Best Actor Oscar for his blood-chilling role as Col. Hans Landa in Inglourious Basterds, the Affordable Care Act was signed into law, and oxycontin was reformulated to be less crushable and deter abuse.
Could that last have something to do with the rise in hepatitis C infections? It’s a tricky question, but one that was addressed fairly thoroughly by this article, appearing in Health Affairs.
The theory goes like this. In 2010, oxycontin is reformulated to make it harder to crush / snort / inject, etc. Abusers of oxycontin move on to heroin, often using the drug intravenously. IV drug use leads to an increase in hepatitis C infections.
And though we’ve had some cohort-study data to support this hypothesis, until this week we didn’t have a broad, national study with appropriate controls. Now we do – so let me walk you through it.
Researchers combined data from the nationally-representative Survey on Drug Use and Health with state-level hepatitis C infection rates from the CDC.
The data were pretty clear - the rates of oxycontin misuse actually decreased after 2010, as intended, but the rate of heroin overdose and hepatitis C infections went up.
But this still isn’t enough to be sure that it was the reformulation that was responsible – after all, a lot happened in 2010. “Sarah Palin’s Alaska” premiered on the discovery channel, for cryin’ out loud.
So the authors went a step farther. They hypothesized that states that used more oxycontin would be disproportionately affected by the oxycontin reformulation. Those states, then, would have a more rapid increase in hepatitis C than states where oxycontin wasn’t as often misused.
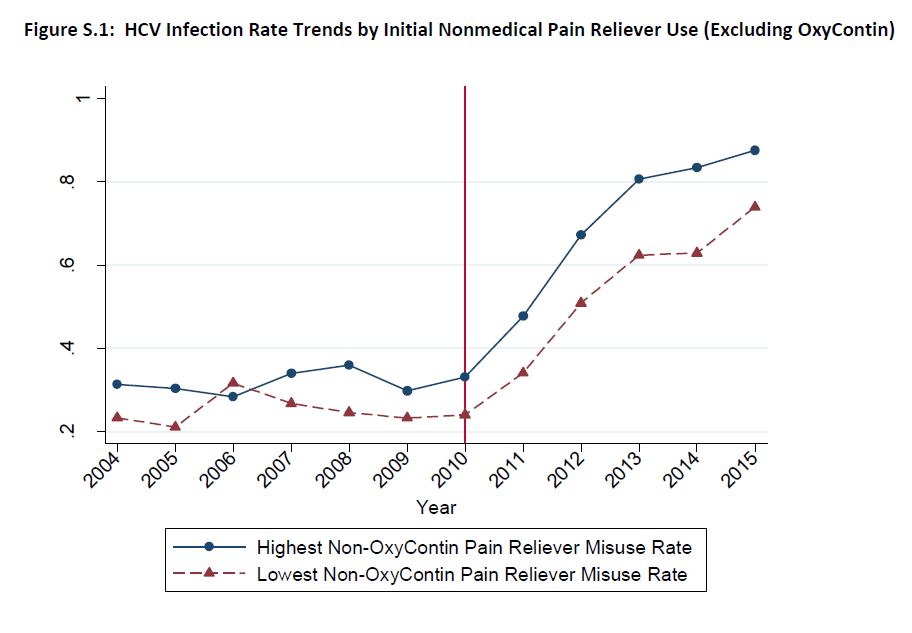
And what they found is visualized here.
Prior to the oxycontin reformulation, the rates of hepatitis C were pretty similar in states where there was a lot of oxycontin use compared to states without a lot of oxycontin use. But after the reformulation, states that had a lot of oxycontin use had a much more dramatic rise in hepatitis C than those that hadn’t been using oxycontin as much.
Still not convinced? They did the same analysis using non-oxycontin narcotics.
Splitting the states in terms of, say, how much hydrocodone they use shows that both groups of states have a similar increase in hepatitis C rates after 2010. This is good evidence that the problem here was the oxycontin reformulation, as opposed to just more opioid abuse in general.
Now we could stop here, shake our heads and tsk tsk a bit about the best laid plans of mice and pharma. Indeed – much of the media covering this study paints the oxycontin reformulation as a failure.
But be careful – there’s a missing data point here.
I would argue that a key outcome is the total number of opioid overdose deaths, not heroin-specific deaths. It is possible – even likely – that the oxycontin reformulation pushed some people to heroin and they subsequently died. It is also possible that it pushed some people to get into rehab. To tease it all apart, we’d want to look at the change in total opioid overdose rates among states with high vs. low exposure to oxycontin.
I asked lead author Dr. David Powell about differences in total overdoses. He wrote
…there isn’t overwhelming evidence that reformulation necessarily increased total overdoses. But, we need to think about the other consequences of broad shifts from prescription opioids to heroin. One of those consequences is a rise in infectious diseases.
In other words, the reformulation may be robbing Peter to pay Paul in terms of deaths, but the risk to public health in general should show us that trying to deter abuse without providing support for addiction treatment is a loss all around.
This commentary first appeared on medscape.com.